Procedures come and go in
the field of cosmetic surgery, and if a given modality makes
it a decade, it probably has merit and is here to stay,
pending a newer technology.

COMMON COMPLICATIONS
|
Laser resurfacing techniques are
probably on a decline as a whole, but not because the laser is
an ineffective modality. The modest decline probably
represents the fact that the novelty has worn off, and that
many people who are candidates for laser resurfacing, have
already been treated. Those whom obfuscate this procedure
point out increased complications and increased recovery, but
for those who have endured the learning curve, there is no
more effective procedure for given indications. I would bet
that most of the clinicians that rebuke laser resurfacing do
not own their own lasers and have had bad experiences with the
procedure. Granted, there are easier procedures with less of a
recovery period, but in my opinion, there is still no
substitute for rhytide effacement in severely actinically
damaged and aged skin.
As the world plugs along
for a noninvasive alternative resurfacing, many of us continue
to rejuvenate our patients with the CO2 laser. There is no
doubt that laser resurfacing patients will have complications,
but is there any cosmetic procedure that produces a result
that has none? For the most part, the spectrum of
complications associated with CO2 laser resurfacing are
predictable and treatable. They can be anticipated and planned
for.
Multiple studies have
consistently documented laser resurfacing complications. Drs.
Alster and Nanni (see for more information) reviewed 500 laser
cases and listed the complications as follows:

PRELASER INFORMED CONSENT CASCADE
|
One can observe that the most severe
complications such as hypertrophic scarring and true
hypopigmentation are indeed rare. Other complications such as
hyperpigmentation and milia formation are, on the other hand,
common.
The best means of dealing
with a complication is to anticipate it. The informed consent
process cannot be overstated.
Cosmetic patients cannot be
overeducated about their prospective procedures. Merely having
an informed consent may protect you in a court of law, but
still lead to disgruntled patients that can dissipate negative
marketing for your practice. A potential problem that is
discussed preoperatively is a sequela, but when it is
discussed postoperatively, it is a complication!
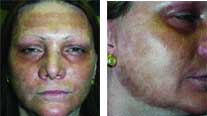
Following laser resurfacing, the
patient developed significant hyperpigmentation at four
weeks posttreatment.
|
Most of us perform cosmetic surgery
every day, but for many patients this will be their first, and
possibly, only procedure. This means that we often assume our
messages about treatment and complications are loud and clear,
because it is so repetitive in our practices. The patients on
the other hand may be so overwhelmed with fear, anxiety,
economics, recovery, etc. that their understanding process is
actually disabled. For this reason, it is imperative to
confront the informed consent process on multiple fronts.
In our office, we have
every patient read and sign a witnessed informed consent. In
addition, we provide them names of patients who have had
similar procedures and can provide communication first hand.
An additional technique
that has proven very valuable is to have every patient view an
in-office PowerPoint show that details his or her procedures.
These shows take only minutes to put together and are
extremely useful.
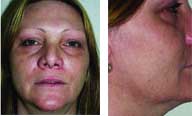
Obagi
skin products were used to clear the hyperpigmentation
over a three-week period. (Photographs courtesy of
Joseph Niamtu, III, D.D.S.)
|
From time to time we have a patient
view the show and he or she cancels the procedure. Although no
one wants to lose a patient, they are doing us a favor because
this patient would be overwhelmed with a complication (or
possibly with the basic procedure) and make your life
miserable until it is resolved.
The final step of our
informed consent process is to have the patient sign a
separate form, which the surgeon reviews with the patient
that, again, lists the possible complications.
This form is much less
encumbered than the procedural informed consent and basically
lists the 10 or 12 possible problems including overtreatment,
undertreatment, demarcation lines, sun avoidance, etc. This
multistep informed consent process has proven invaluable when
dealing with postlaser complications. Again, it is important
to remember that merely escaping a lawsuit is not a win if
unhappy patients defame your reputation. Most cosmetic
practices are about marketing, and negative marketing is a
serious reality.
It is beyond the scope of
this article to discuss all the complications of laser
resurfacing, so we will focus on two of the more common
problems, prolonged erythema and postinflammatory
hyperpigmentation.
Prolonged erythema
I have had some patients with
excellent postlaser results, but then be unhappy because there
is a demarcation line where the laser stopped.
Technically, this is
relative hypopigmentation in that there is no actual
melanocytic damage, but there exists a color difference
between the rejuvenated face and untreated neck skin. It is
very important to inform the patient that the laser must stop
somewhere and traditionally it is the mandibular shadow.
We show them the lateral
skin of their biceps, which is usually sundamaged and darker
when compared to the medial biceps skin. This is usually more
protected and like rejuvenated or younger skin, it is lighter.
Usually, this demarcation
will fade and blend with the neck skin, but we also give the
patient an option of simultaneous TCA neck peel to better
blend the laser treatment.
Not a complication, but it
still looks bad
Prolonged erythema is not
truly a complication, but is probably the most unpopular
sequella of CO2 laser resurfacing. Postlaser redness can last
weeks or months (average 2 to 4.5 months, and is frequently
unnoticeable at 12 to 16 weeks).
Since the erythema is a
healing response, one cannot do much to alter its course and
some patients simply remain red longer than others.
I show my patients pictures
of the extremes of erythema and if their redness resolves
quicker, I am a hero and if it does not, "I told them so." I
have been recently doing an informal trial of Carrasmart Gel
wound dressing (Carrington Laboratories, Inc., Irving, Texas),
which seems to decrease postoperative erythema. This product
contains acemannan hydrogel and is used for burns and stasis
ulcers. It is applied topically as a coating and replenished
continually for protection.